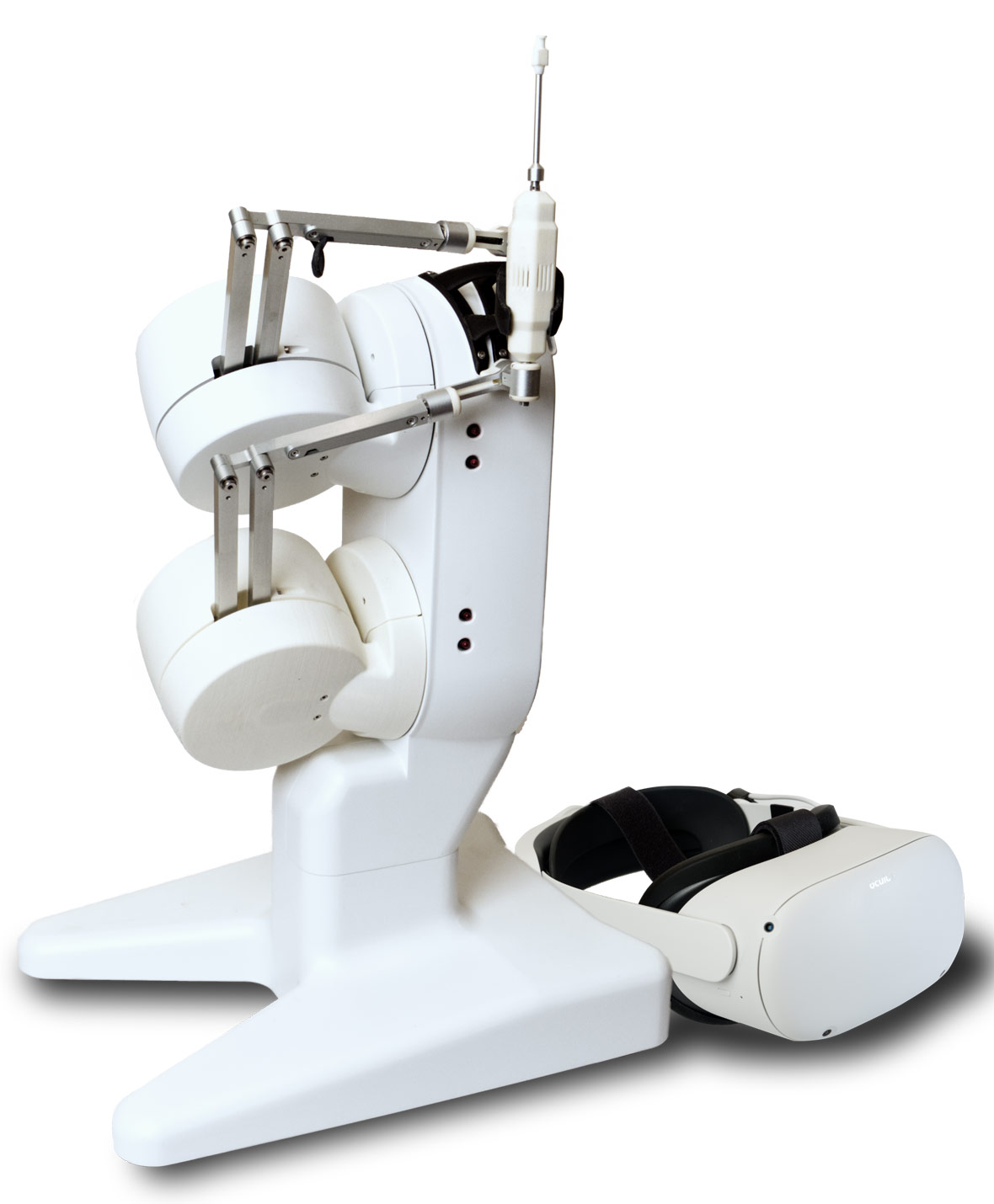
Practice your procedure virtually, with stunning realism – beforehand!

CT scan of the patient is uploaded to Marion.

Virtual reality environment of the particular surgery is created.

Practice the procedure and improve accuracy on the actual patient with our patent-pending haptics.
Trusted by:
Validation
Marion Surgical Patent
Granted Q2 2022
A system for simulating surgical procedures on a patient anatomy in a virtual environment with haptic feedback.
- Publication Number: WO / 2019/218081
- Publication Date: 21.11.2019
- International Application No.: PCT / CA2019 / 050675
- International Filing Date: 05/17/2019
- Estimated time to Be Granted: Q2 2022
The problem in numbers:
Million Patients
undergo surgery
worldwide each year
Million Patients
Suffer from complications
during and following surgery
Million People
Die as a result
$1.3B
Cost of preventable mistakes
in surgery every year
“This is the future: this simulator allows you to pre-operatively practice how a particular patient specific case will go.”
Jason Young Lee MD, MHPE, FRCSC
Assistant Professor, Division of Urology, Department of Surgery, Toronto General Hospital
University of Toronto, Urology Residency Program Director
Associate Member, Institute of Medical Science